Urethral stricture
Urethral stricture presents various degrees of narrowing or complete obliteration of urethral channel. Any part of urethra may be affected. Patient has difficulty to urinate and empty the bladder. Urethral stricture presents a huge functional, psychological, social and sexual problem for the patient.
Urethral strictures can be caused by:
– trauma (straddle injury, pelvic fracture),
– infection (gonococcal, chlamidia urethritis),
– dermatologic disease (Lichen sclerosis),
– congenital anomaly of the penis (hypospadias),
– iatrogenic treatment (catheterization, endoscopic procedures).
Moreover, some urethral strictures have unknown origin and they are called idiopathic.
Patient usually has difficulty to empty the bladder, painful urination, weak urine stream, spraying of urine, dribbling, urinary incontinence, urinary tract infections and decreased ejaculation force. Sometimes symptoms may be absent.
When the medical history reveal symptoms that are suggestive of urethral stricture, additional specific diagnostic examination may be helpful in further evaluation. Special X-rays combined with contrast filling of the urethra can demonstrate the site and severity of a stricture. Visual examination of the urethra by a thin optic instrument may be needed to assess the stricture. Tests to determine the flow rate of urine are usually advised. The flow rate is much reduced if the stricture is present.
Treatment
The treatment options for urethral stenosis are: dilatation, endoscopic incision (urethrotomy) and surgical reconstruction (urethroplasty).
1. Dilatation procedure presents stretching of the stricture using progressively larger metal dilators. Dilatation is rarely a cure and needs to be periodically repeated. Pain, bleeding, infection and creating of “false passage” are the main problems associated with dilation procedures.
2. Urethrotomy procedure is incising narrowed segment of urethra by knife blade or laser inserted by endoscopic instrument. This therapeutic option can be successful for very short urethral strictures in specific part of the urethra. Urethrotomy, as well as dilatation, can cause excessive damage of the urethral tissue and actually aggravate urethral stricture.
3. Open surgical reconstruction of urethra presents contemporary treatment of urethral strictures. Various techniques of open repair are used. Urethral channel can be reconstructed or replaced by one or two stage procedures. The type of repair depends on the characteristics of the stricture (location, length and severity) and no single repair is appropriate for all strictures. Anastomotic repair includes removal of scarred urethral segment and reattachment of urethral stumps. This procedure is reserved for short urethral strictures located in posterior part of urethra. Narrowed urethral segment can be augmented by buccal mucosa graft or penile skin flap. Completely obliterated longer urethral segment can be replaced by combined buccal mucosa graft and penile skin flap as one stage procedure. Two-stage urethral reconstruction includes placement of buccal mucosa graft as first stage procedure and tubularization into neourethra as second stage six months later.
All stated surgical procedures are performed in our center with high success rate. The best quality silicon urethral catheters are used for urethral modeling and stenting. Catheters are left for 7 to 14 days, depending of the type of urethral stricture and type of procedure. Suprapubic urinary tube can be used to enable better and faster healing of the reconstructed urethra. If buccal mucosa graft is harvested, donor site defect is usually closed directly and it heals within 3-5 days.
Belgrade Center for Genital and Reconstructive Surgery® is always in search for new and better solutions for the treatment of urethral strictures, as well as other entities, such as urethral diverticulum. The long-term follow up of these patients enables the best assessment of the achieved surgical results. Constant comparison of our results with the results from different medical centers around the world as well as exchange of knowledge and experience allows us to establish the best surgical option for our patients.
CASE 1
Long iatrogenic anterior urethral stricture

Echosonographic appearance

Intraoperative appearance

Dorsal buccal mucosa graft urethroplasty

Dorsal buccal mucosa graft urethroplasty

Echosonographic appearance after surgery – adequate lumen is achieved
CASE 2
Staged repair of anterior urethral stricture – combined buccal mucosa and full thickness skin graft urethroplasty

Buccal mucosa graft urethroplasty

Full thickness skin graft urethroplasty

Graft tubularization

Graft covering

Echosonographic appearance after surgery – adequate lumen is achieved
CASE 3
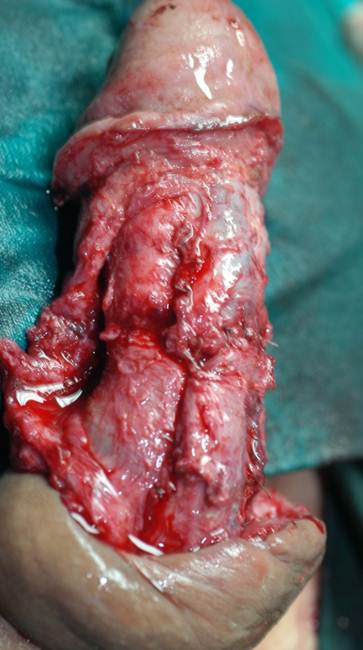
Penile / urethral trauma

Intraoperative appearance

Intraoperative appearance

Dorsal “roof” augmented urethroplasty

Dorsal “roof” augmented urethroplasty
Venous graft corporoplasty

Venous graft corporoplasty

Appearance after surgery
CASE 4
Long bulbar urethral stricture wuth spongiofibrosis

Echosonographic appearance

Intraoperative appearance

Buccal mucosa graft urethroplasty

Dorsal onlay buccal mucosa graft urethroplasty

Echosonographic appearance two years after surgery – adequate lumen
CASE 5
Straddle injury of bulbar urethra

Short segment – dense spongiofibrosis

Proximal urethral mobilisation

Anastomotic repair of urethra

Echosonographic appearance two years after surgery – adequate lumen
CASE 6
Proximal bulbar stricture after TURP

Echosonographic appearance

Dorsal inlay buccal mucosa graft urethroplasty

Ventral onlay buccal mucosa graft urethroplasty

Satisfactory patent lumen one year after surgery
CASE 7
Posterior urethral stricture

Anterograde VCUG appearance

Retrograde VCUG appearance

Dissection of proximal opening of distal urethra and anastomosis
1. Djordjevic ML. Graft surgery in extensive urethral stricture disease. Curr Urol Rep. DOI: 10.1007/s11934-014-0424-3.
2. Djordjevic M., Milosevic A., Acimovic M., Kojovic V. Anterior urethral substitution by combined buccal mucosa graft and penile skin flap. Eur Urol Suppl 2011;10(9);580.
3. Djordjevic ML, Kojovic V, Bizic M, Majstorovic M, Vukadinovic V, Korac G. “Hanging” of the buccal mucosal graft for urethral stricture repair after failed hypospadias.J Urol. 2011 Jun;185(6 Suppl):2479-82. Epub 2011 Apr 27.
4. Kojovic V, Majstorovic M, Bizic M, Ducic S, Djordjevic M, Urethral stricture repair after failed hypospadias by hanged ventral buccal mucosa graft, 42nd Annual Meeting of Pacific Association of Pediatric Surgery,Hong Kong, 2009, p120, (P076)